Why Decompression Sickness Expert Diagnosis Can't Wait
Decompression sickness expert diagnosis is a time-sensitive, purely clinical process — there is no single lab test or scan that confirms it. If you or a patient surfaces from a dive with unusual symptoms, here's what you need to know right away:
Quick Answer: Key Steps for Decompression Sickness Expert Diagnosis
- Recognize the timing — 50% of DCS symptoms appear within 1 hour of surfacing; 90% appear within 6 hours
- Identify the symptom type — joint pain, numbness, neurological deficits, dizziness, or skin mottling are the most common signs
- Administer 100% oxygen immediately — this is the critical first-aid step before reaching a hyperbaric facility
- Call a dive medicine emergency line — such as Divers Alert Network (DAN) at 919-684-9111 for specialist guidance
- Reach a hyperbaric chamber fast — recompression therapy is the gold standard treatment and also serves as a diagnostic confirmation
Decompression sickness (DCS) is rare — estimated at roughly 1 in 10,000 dives — but when it happens, the window for effective treatment is narrow and the consequences of delay can be permanent.
What makes it especially tricky is that DCS doesn't always look the same. Symptoms can range from mild joint aching to paralysis, and they can build slowly — making it easy for divers to dismiss early warning signs. As one guiding principle in dive medicine puts it: any symptom appearing after a dive should be considered pressure-related until proven otherwise.
DCS falls under a broader umbrella called decompression illness (DCI), which also includes arterial gas embolism (AGE) — a distinct but related condition that requires the same urgent response. Telling them apart matters clinically, but both demand immediate expert evaluation.
Adding another layer of difficulty: 86% of hyperbaric chambers reporting to Divers Alert Network see fewer than 10 DCI cases per year. True clinical expertise in this field is genuinely rare, which is exactly why knowing where to turn — and fast — is so important.
Navigating Decompression Sickness Expert Diagnosis and Clinical Presentation
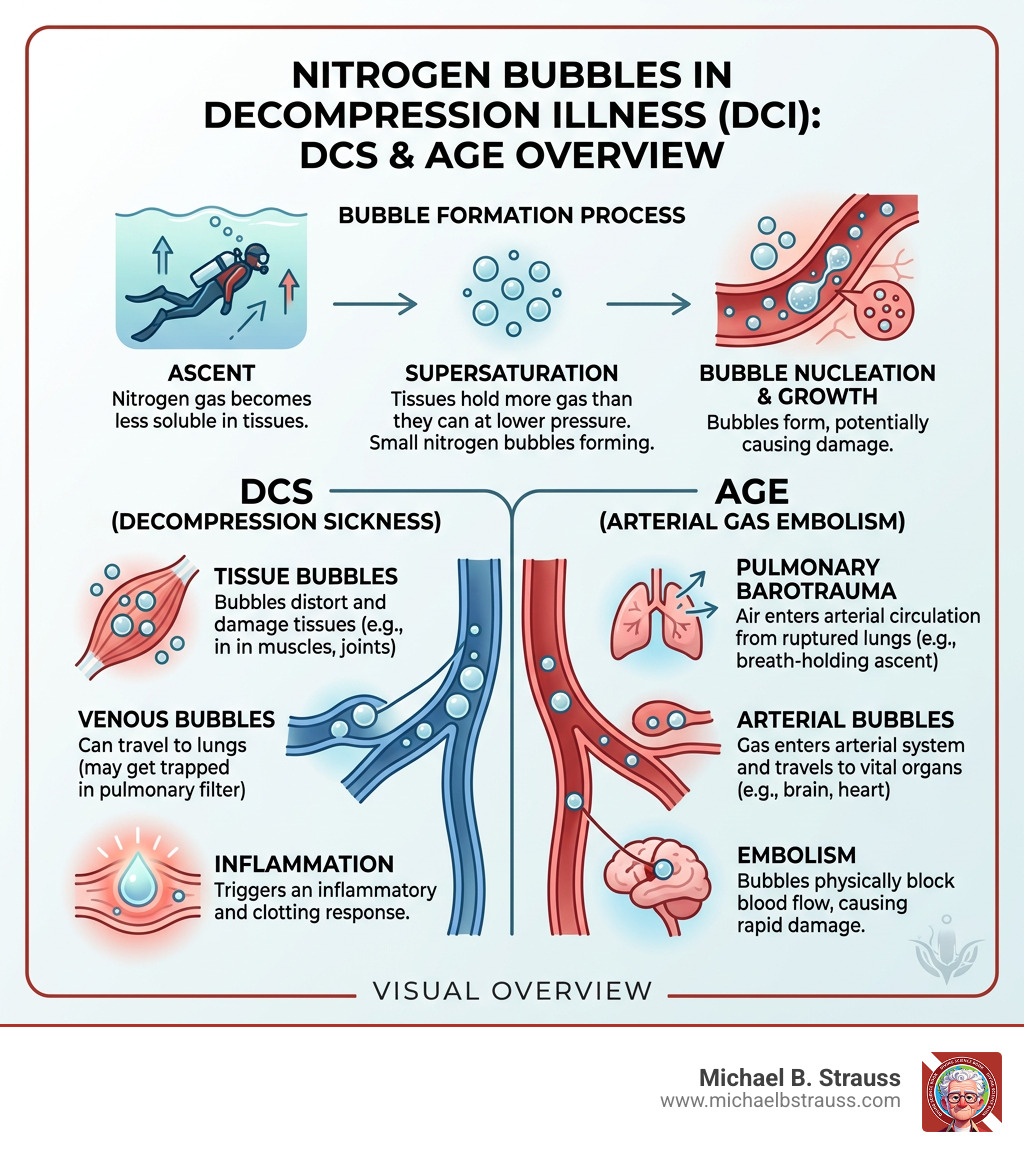
When we talk about decompression sickness expert diagnosis, we have to look past the surface. While most people think of DCS as just "bubbles in the blood," those bubbles are actually the gateway to a complex cascade of biological trouble.
The pathophysiology starts with supersaturation. As we dive, the increased ambient pressure causes inert gases (usually nitrogen) to dissolve into our body tissues. If we ascend too quickly, those gases can't stay in solution. They form bubbles—a process called bubble nucleation—which can distort tissues, block blood flow, and trigger an inflammatory response.
Comparing the "Bends": Type 1 vs. Type 2 DCS
To make things clearer for clinical evaluation, experts often categorize DCS into two main types. This helps us prioritize treatment based on the severity of the organ systems involved.
| Feature | Type 1 DCS (Mild) | Type 2 DCS (Serious) |
|---|---|---|
| Primary Systems | Musculoskeletal, Skin, Lymphatic | Neurological, Inner Ear, Cardiopulmonary |
| Common Signs | Joint pain, itching, localized swelling | Numbness, weakness, vertigo, "the chokes" |
| Urgency | High (requires evaluation) | Critical (emergency recompression) |
| Frequency | Represents about 85% of cases | Less common but far more dangerous |
Because the symptoms can be idiosyncratic—meaning they present differently in everyone—a Scientific research on DCS clinical aspects is vital to understanding how these cases evolve in the real world.
Recognizing Symptoms for Decompression Sickness Expert Diagnosis
The timing of symptoms is one of our best diagnostic tools. While some divers expect to feel "bent" the moment they hit the surface, the reality is more gradual. Only about half of patients show symptoms within the first hour. By the six-hour mark, 90% have manifested signs, but we’ve seen cases appear up to 36 hours later.
According to Scientific research on DCS manifestations, here is how symptoms generally rank by frequency:
- Pain (Joints and Muscles): Reported in nearly two-thirds of cases. It often feels like a deep, dull ache that doesn't get worse when you move the joint.
- Numbness and Paresthesia: Also seen in about two-thirds of cases, often signaling neurological involvement.
- Constitutional Symptoms: Fatigue, headache, or a general feeling of malaise occur in approximately 40% of cases.
- Dizziness and Vertigo: Seen in about 20%, often indicating inner-ear DCS.
- Motor Weakness: Occurring in 20% of cases, this is a major red flag for spinal cord involvement.
- Cutaneous (Skin) Manifestations: About 10% of divers experience itching or rashes. A specific mottled appearance called cutis marmorata is particularly concerning, as it often precedes more severe neurological symptoms.
Differential Diagnosis: Distinguishing DCS from AGE and Barotrauma
One of the hardest parts of decompression sickness expert diagnosis is ruling out "mimics." Not every post-dive problem is DCS. We have to look at the Expert review on differential diagnosis to distinguish between various conditions:
- Arterial Gas Embolism (AGE): Usually occurs within minutes of surfacing. It often involves a sudden loss of consciousness or stroke-like symptoms and is caused by lung over-expansion (barotrauma) rather than nitrogen saturation.
- Immersion Pulmonary Edema (IPE): This involves fluid in the lungs and can cause cough and shortness of breath, but it isn't caused by bubbles.
- Inner Ear Barotrauma: This can cause vertigo and hearing loss similar to inner-ear DCS, but it usually happens due to difficulty equalizing during the descent or ascent.
- Nitrogen Narcosis: While this happens at depth and resolves upon ascent, it can sometimes be confused with the early stages of a complex DCI event.
- Stroke or Heart Attack: Especially in older divers, we must ensure we aren't mistaking a standard medical emergency for a diving-related one.
The Role of Risk Factors in Decompression Sickness Expert Diagnosis
Why does one diver get bent while their buddy, on the exact same profile, stays perfectly fine? This is the "idiosyncratic" nature of the disease. Several factors can increase your risk:
- Dive Profiles: Deep dives, long durations, and rapid ascents are the primary drivers.
- Dehydration: Thicker blood (higher hematocrit) can slow down nitrogen elimination.
- Cold Water: Diving in cold water but having a warm shower immediately after can trigger bubble formation as tissues warm up and gas expands.
- Patent Foramen Ovale (PFO): This is a small hole in the heart that didn't close after birth. It can allow venous bubbles to bypass the lungs (the body’s natural bubble filter) and go straight to the brain or spine. Research on PFO and DCS risk shows it is a significant factor in "undeserved" DCS cases.
- Body Mass Index (BMI): Since nitrogen is highly soluble in fat, higher body fat percentages can lead to more nitrogen storage, though the data on this as a primary risk factor is still debated among experts.
Gold Standard Treatments and Expert Management Protocols
Once a decompression sickness expert diagnosis is made, the priority shifts to recompression. The goal is simple: shrink the bubbles and force the nitrogen back into solution while flooding the tissues with life-saving oxygen.

Because experts are rare, we rely on standardized US Navy Diving Manual protocols. These "Treatment Tables" dictate exactly how deep the chamber should go and how much oxygen the patient should breathe.
Immediate First Aid and Hyperbaric Oxygen Therapy (HBOT)
Before you ever reach a chamber, first aid is critical. The Expert review of pre-hospital management emphasizes that 100% normobaric oxygen is the single most important intervention. It creates a "pressure gradient" that helps nitrogen leave the tissues faster.
- Oxygen Administration: Use a close-fitting mask to ensure the highest concentration possible.
- Fluid Management: If the diver is conscious, oral rehydration is helpful. If they are severe, IV isotonic fluids (like Normal Saline) are preferred. Avoid sugar-heavy drinks.
- Positioning: Keep the patient horizontal. The old "Trendelenburg" (head-down) position is no longer recommended as it can cause brain swelling.
- US Navy Table 6: This is the "workhorse" of hyperbaric medicine. It involves a treatment lasting about 4 hours and 45 minutes at a simulated depth of 60 feet (2.8 ATA).
Evidence-Based Prevention and Long-Term Prognosis
The best way to handle DCS is to never get it in the first place. We recommend several layers of safety:
- Conservative Diving: Don't push your dive computer to the limit.
- Safety Stops: A 3-to-5-minute stop at 15 feet is essential for letting off excess nitrogen.
- Ascent Rates: Keep it slow—no faster than 30 feet per minute.
- Nitrox Benefits: Using Enriched Air Nitrox (high oxygen, low nitrogen) while following air tables provides a massive safety buffer.
- Hydration: Drink plenty of water before and between dives.
Consulting Dive Medicine Experts for Recovery
Most divers recover fully if treated promptly. However, delays can lead to long-term issues like permanent nerve damage or dysbaric osteonecrosis (bone death caused by interrupted blood flow).
When navigating the recovery process, consulting a dive medicine expert is non-negotiable. Dr. Michael B. Strauss has dedicated his career to diving science and the evaluation and management of pain-related medical problems of diving. Understanding why and at what sites decompression sickness can occur is a core part of his research.
For those looking to dive deeper into the mechanics of the sport, his books on decompression science are essential for understanding how to stay safe.
Recovery isn't just about the chamber; it's about a managed return to the water. We follow the latest Scientific research on inner ear DCS recovery and consensus guidelines from organizations like the Undersea and Hyperbaric Medical Society (UHMS) to ensure that when you do get back in the water, you do so with a clean bill of health.
Final Expert Tip: Never ignore "the niggles." If you feel a weird ache or a patch of skin feels numb after a dive, don't wait for it to get worse. Early intervention is the difference between a quick recovery and a life-altering injury. Stay safe, dive conservative, and always keep an emergency contact for a dive expert in your kit.
To get or buy the book Diving Science Revisited, visit this link: https://www.bestpub.com/view-all-products/product/diving-science-revisited/category_pathway-48.html
DISCLAIMER: Articles are for "EDUCATIONAL PURPOSES ONLY", not to be considered advice or recommendations.






