Can You Scuba Dive with Asthma? What You Need to Know First

Scuba diving asthma inhaler use is one of the most searched — and most misunderstood — topics in dive medicine. Here's the short answer:
- Do not use a pressurized inhaler underwater. Depth changes pressure, which makes inhaler delivery unreliable and potentially dangerous.
- Do use your inhaler before diving — ideally 30 minutes before entering the water.
- Keep your inhaler on the dive boat, within easy reach for post-dive emergencies.
- Do not dive if you used a rescue inhaler within the last 48 hours.
- Well-controlled asthma is not an automatic ban from diving — but it does require medical clearance.
Asthma affects roughly 1 in 13 Americans. And here's something that might surprise you: studies show that asthma is just as common among scuba divers as it is in the general population. Many people with asthma are already diving — some without even telling their instructors.
That's a problem.
Scuba diving creates a unique set of respiratory challenges. The compressed air you breathe through a regulator is cold and dry — two of the most common asthma triggers. Add in physical exertion, depth-related pressure changes, and the stress of an unfamiliar environment, and you have a situation that demands careful planning.
The good news? Well-controlled asthma does not have to keep you out of the water. Research consistently shows that asthmatics with stable, well-managed conditions can dive safely — if they follow the right protocols and get proper medical clearance.
This guide walks you through exactly how to do that.
Basic scuba diving asthma inhaler terms:
Managing Your Scuba Diving Asthma Inhaler and Risks
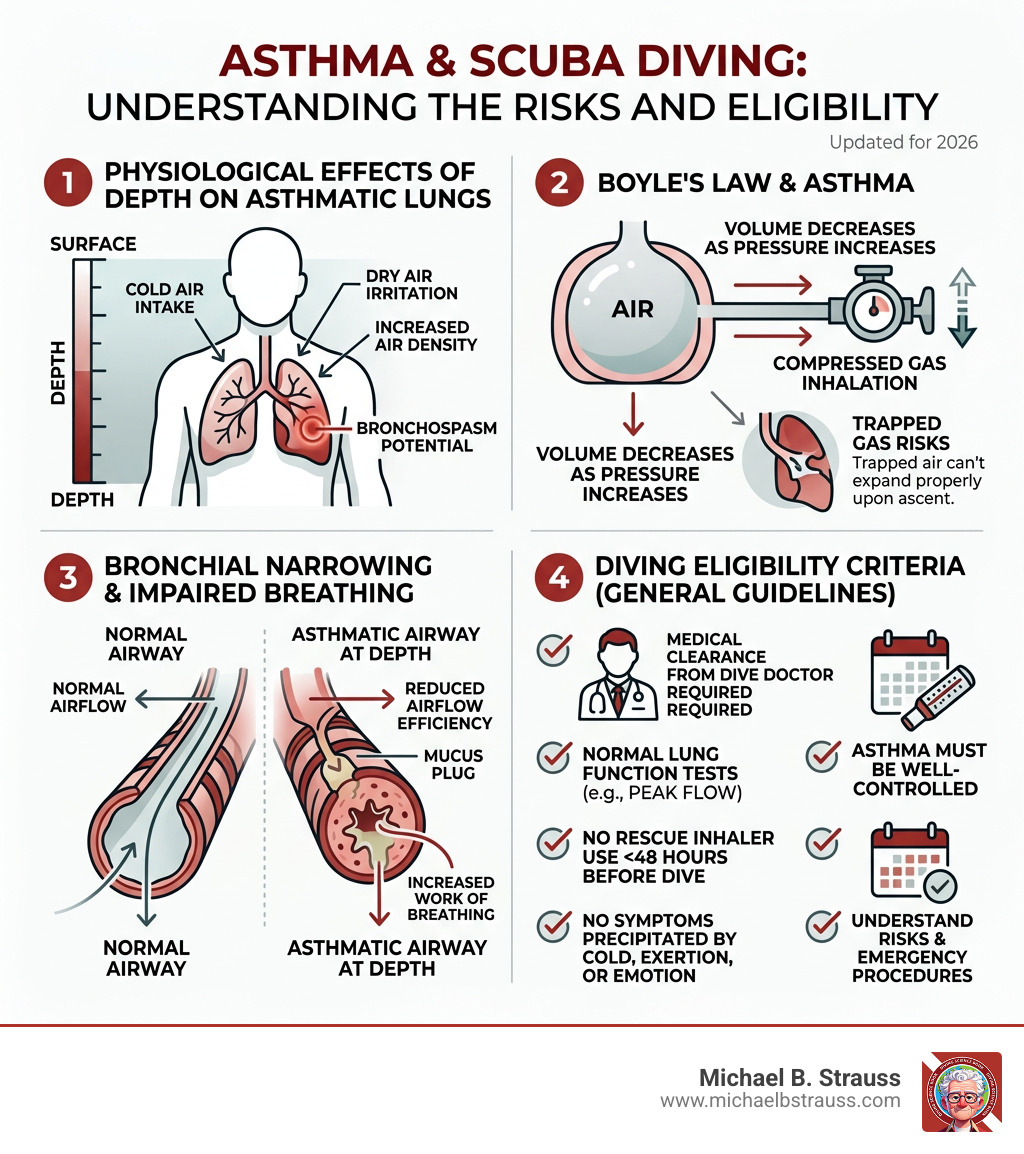
When we talk about asthma and diving, we aren't just talking about being short of breath. We are talking about the physics of the ocean and how they interact with your anatomy. The primary concern for any diver with asthma is the risk of pulmonary barotrauma (lung over-expansion injury).
According to Boyle’s Law, as a diver ascends and the surrounding pressure decreases, the air inside the lungs expands. In a healthy lung, this air is exhaled normally. However, asthma causes bronchial narrowing and excess mucus production. This can lead to "gas trapping," where air becomes stuck behind a narrowed or blocked airway. As you surface, that trapped air expands, potentially causing the air sacs (alveoli) to rupture. This can lead to a collapsed lung (pneumothorax) or, more dangerously, an Arterial Gas Embolism (AGE), where air bubbles enter the bloodstream and travel to the brain.
Despite these theoretical risks, epidemiological data suggests that the danger for well-controlled asthmatics may be lower than once feared. A survey of 279 asthmatic divers participating in over 56,000 dives showed that while 11 cases of decompression sickness were reported, the overall risk was comparable to the general diving population. To stay safe, it is vital to understand the condition through resources like MedlinePlus asthma information and consult scientific research on asthma and diving safety before hitting the water.
Why You Shouldn't Use a Scuba Diving Asthma Inhaler Underwater
It is a common question: "Can I just bring my scuba diving asthma inhaler with me on the dive?" The answer is a firm no. Attempting to use a Metered Dose Inhaler (MDI) at depth is fraught with mechanical and physiological peril.
First, pressurized inhalers are not rated for underwater use. The physics of depth affects the propellant inside the canister. At 30 meters, the ambient pressure is four times that of the surface. This can cause the delivery mechanism to fail or, worse, deliver a highly concentrated and variable dose that could lead to an accidental overdose.
Furthermore, the logistics are nearly impossible. Trying to coordinate the "press and breathe" technique while holding a regulator or wearing a full-face mask is a recipe for panic. If you are symptomatic enough to need a rescue inhaler underwater, you are already in a life-threatening situation. The priority should be a calm, controlled ascent, not struggling with a device that wasn't designed for the abyss.
Pre-Dive Protocols for Your Scuba Diving Asthma Inhaler
Preparation starts long before you put on your fins. If you have been cleared to dive, a standard protocol involves using your "reliever" or rescue inhaler (such as Albuterol) approximately 30 minutes before the dive. This helps ensure your airways are as open as possible to combat the dry, cold air from your tank.
Once you are on the boat, your scuba diving asthma inhaler should be stored in a dry bag, clearly labeled, and placed where the divemaster or your buddy can find it instantly. Communication is key. You must tell your dive buddy about your condition and establish hand signals for chest tightness or breathing discomfort. We recommend reviewing the Evaluation and Management of Pain-Related Medical Problems of Diving for a deeper look at how medical issues are handled in a diving context.
Medical Clearance and Fitness to Dive (FTD)
You cannot "self-clear" for diving if you have asthma. A formal Fitness to Dive (FTD) evaluation by a physician trained in hyperbaric medicine is mandatory. During this evaluation, doctors look for several key indicators:
- Spirometry: This measures how much air you can inhale and exhale, and how fast. Specifically, doctors look at the FEV1/FVC ratio. A ratio of at least 0.8 (80%) is generally required.
- Peak Flow Monitoring: You should be able to demonstrate that your peak expiratory flow (PEF) is stable and within 10% of your personal best.
- Exercise Challenge: Since diving is a physical activity, a doctor may perform a "stress test" where you exercise and then have your lung function re-tested to ensure you don't suffer from exercise-induced bronchospasm.
- Reversibility Testing: This checks if your lung function improves significantly after using a bronchodilator, which helps determine the "twitchiness" of your airways.
Organizations like the Divers Alert Network (DAN), the UK Diving Medical Committee (UKDMC), and the South Pacific Underwater Medicine Society (SPUMS) all provide guidelines that emphasize individual assessment over blanket bans.

Essential Precautions for Asthmatic Divers
Diving with asthma is about risk mitigation. We want to minimize the triggers that could cause a bronchospasm while we are at depth. One of the most overlooked factors is hydration. Compressed air is extremely dry—often having less than 0.1% humidity. This can dry out the mucus in your airways, making them more irritable. Drinking plenty of water before and after your dive is essential.
Environmental choices also matter. We strongly recommend that asthmatic divers stick to warm, tropical waters. Cold water is a major trigger for asthma attacks and increases the physical work of breathing. Additionally, always plan for a slow, conservative ascent. The last 5 to 10 meters are the most critical, as this is where the greatest proportional pressure changes occur.
Monitoring Peak Flow and Triggers
A responsible asthmatic diver should keep a peak flow diary for at least two weeks leading up to a dive trip. This gives you a baseline of what "normal" looks like for you.
The "48-hour rule" is a gold standard in the industry. If you have needed your rescue scuba diving asthma inhaler within the 48 hours preceding a dive, or if your peak flow is more than 10-15% below your personal best, you must stay on the boat. It’s not worth the risk.
| Asthma Severity | Diving Eligibility | Typical Requirements |
|---|---|---|
| Mild Intermittent | Generally Fit | No symptoms <1/week; stable peak flow |
| Mild Persistent | Often Fit | Well-controlled with daily preventer meds |
| Moderate Persistent | Case-by-Case | Requires rigorous exercise/stress testing |
| Severe Persistent | Usually Contraindicated | High risk of gas trapping and barotrauma |
When to Abort the Dive
Knowing when to call it quits is the mark of an experienced diver. If you feel any of the following, you should signal your buddy and begin a controlled ascent immediately:
- Unexpected shortness of breath.
- Audible wheezing.
- A "tight" sensation in the chest.
- Increased anxiety or a feeling of impending panic.
Panic is the enemy of the asthmatic diver. If you feel a "tightness" starting, stop moving, find a stable piece of rock (if safe) or hover, and focus on slow, deep exhalations. Do not bolt for the surface. A rapid ascent while having a bronchospasm is the most direct path to a lung over-expansion injury.
Conclusion and Expert Safety Resources
Diving is a sport of discipline and awareness. For those of us with asthma, that discipline just happens to include a few extra steps. By working closely with a dive-knowledgeable physician, maintaining a strict pre-dive protocol, and being honest about our symptoms, we can explore the underwater world with confidence.
Dr. Michael B. Strauss has spent a career dedicated to the science of diving safety. His insights into the physiological demands of the underwater environment are essential for anyone looking to push their limits safely. For those interested in the deeper mechanics of how our bodies respond to the pressure of the deep, we highly recommend exploring his diving science books.
The goal of every dive is to return to the surface safely. If you manage your scuba diving asthma inhaler use correctly and respect the limits of your body, you can continue to breathe easy while exploring the wonders of the ocean. For more information on navigating the complexities of dive medicine, visit michaelbstrauss.com/diving-science.
To further your knowledge of diving medicine and safety, get or buy the book from this link: https://www.bestpub.com/view-all-products/product/diving-science-revisited/category_pathway-48.html
DISCLAIMER: Articles are for "EDUCATIONAL PURPOSES ONLY", not to be considered advice or recommendations.






