A New Frontier in Minimally Invasive Surgery
Underwater surgery techniques are a approach to minimally invasive procedures, using fluid immersion instead of traditional gas insufflation.
Core Underwater Surgery Techniques:
- U-EMR (Underwater Endoscopic Mucosal Resection) - Uses water's buoyancy to lift tissue without injections
- U-ESD (Underwater Endoscopic Submucosal Dissection) - Provides clearer visualization for precise tissue removal
- SCUBA Technique - Brain surgery method for removing blood clots with continuous irrigation
- U-POEM - Treats swallowing disorders using fluid-filled environments
- U-EFTR - Full-thickness tissue removal in water-immersed cavities
The concept is simple: filling body cavities with water or saline creates buoyancy effects that naturally lift tissues, making it easier to see and operate without injections.
Dr. Binmoeller first described this in 2012, noting that "water immersion causes mucosal and submucosal layers to lift due to the antigravity effect of submucosal fat tissue." This breakthrough has since expanded across multiple surgical specialties.
Compared to traditional gas insufflation, which can cause complications and limit visibility, underwater techniques offer:
- Better visualization through the 1.3 refractive index of water
- Natural tissue separation without chemical injections
- Improved hemostasis (bleeding control)
- Reduced thermal damage through heat-sink effects
From gastroenterology to neurosurgery, these methods are improving complex procedures. For example, U-EMR achieves higher success rates for certain lesions, and the SCUBA technique has helped 47 patients with brain hemorrhages achieve an average 88.2% clot removal rate.

A Deep Dive into Key Underwater Surgery Techniques
Imagine a surgeon operating not in the ocean, but inside the human body using water-filled spaces. These underwater surgery techniques are some of the most innovative approaches in modern medicine, where fluid replaces gas to create superior surgical conditions. The water environment offers incredible advantages, changing how we approach complex medical procedures.
Underwater Endoscopic Mucosal Resection (U-EMR): A Foundational Underwater Surgery Technique
Underwater Endoscopic Mucosal Resection (U-EMR) is a foundational underwater surgery technique. Instead of injecting saline to lift a lesion, U-EMR fills the entire cavity with water. The buoyancy effect naturally lifts the target tissue away from the muscular wall due to the antigravity properties of submucosal fat—the "floating mucosa" effect.
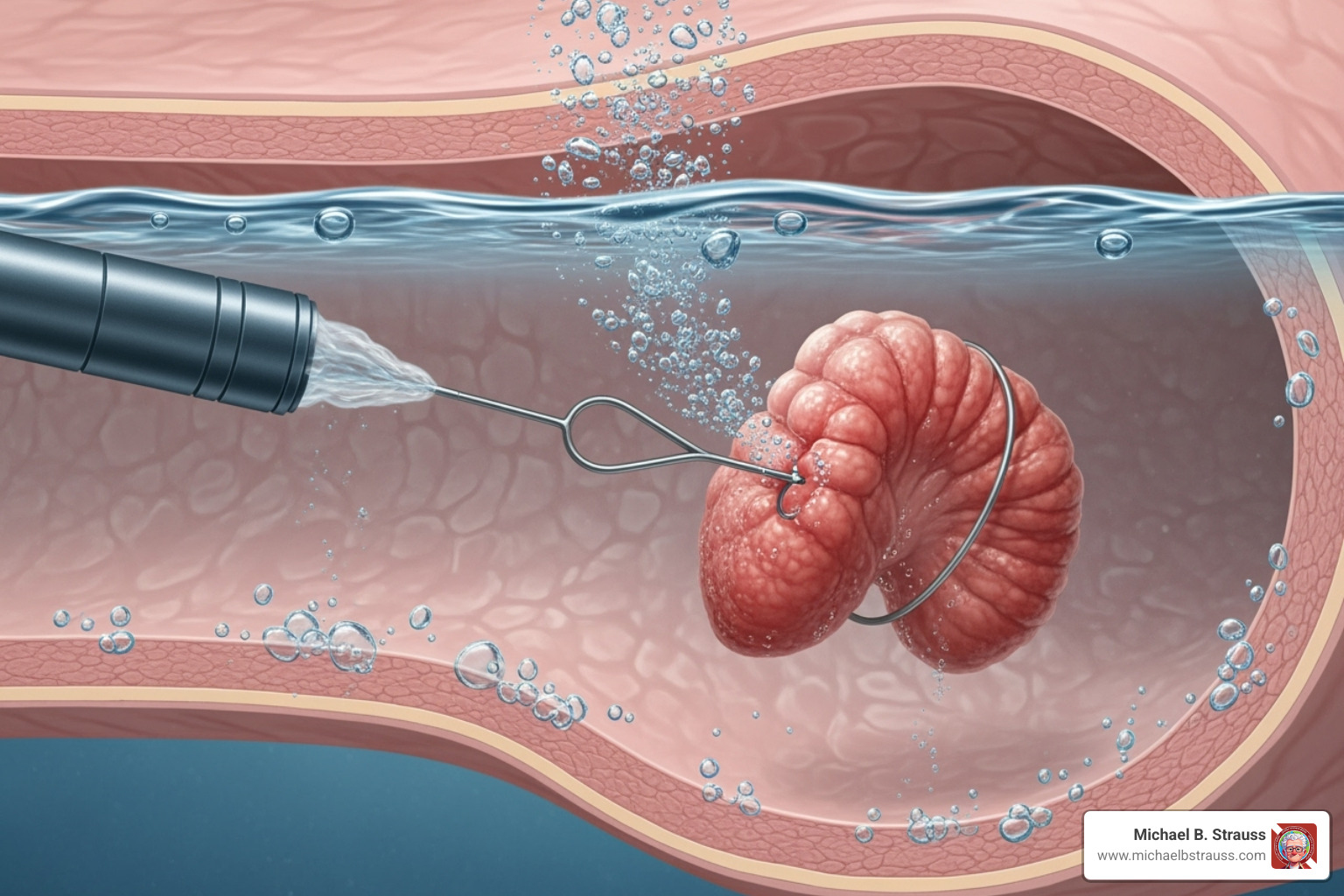
The advantages are significant. Improved visualization comes from water's 1.3 refractive index, making everything clearer. Better hemostasis occurs as the fluid dissipates heat from surgical tools, reducing thermal damage. Best of all, no submucosal injection is needed, eliminating related complications.
The results are compelling, especially for colonic lesions. Research shows U-EMR achieves higher R0 resection rates (69% vs. 50%) and en-bloc resection rates (89% vs. 75%) for lesions between 10-20mm compared to conventional methods. For larger lesions (20-40mm), U-EMR still outperforms with en-bloc rates of 33.3% versus 18.4%.
However, for duodenal lesions, U-EMR shows lower en-bloc and R0 resection rates, reminding us that outcomes vary by anatomical location.
Comparison Table: U-EMR vs. Conventional EMR for GI Lesions
| Feature/Outcome | Colonic Lesions (U-EMR vs. Conventional EMR) | Duodenal Lesions (U-EMR vs. Conventional EMR) |
|---|---|---|
| En-bloc Resection | Higher rates with U-EMR | Lower rates with U-EMR |
| R0 Resection | Higher rates with U-EMR | Lower rates with U-EMR |
| Submucosal Injection | Not required with U-EMR | Not required with U-EMR |
| Visualization | Improved with U-EMR | Improved with U-EMR |
| Hemostasis | Improved with U-EMR | Improved with U-EMR |
Scientific research on U-EMR for colorectal polyps
Advancing the Field with Underwater Endoscopic Submucosal Dissection (U-ESD)
While U-EMR lifts and snares tissue, Underwater Endoscopic Submucosal Dissection (U-ESD) focuses on precision cutting in a fluid environment. It's like performing microsurgery in an aquarium.
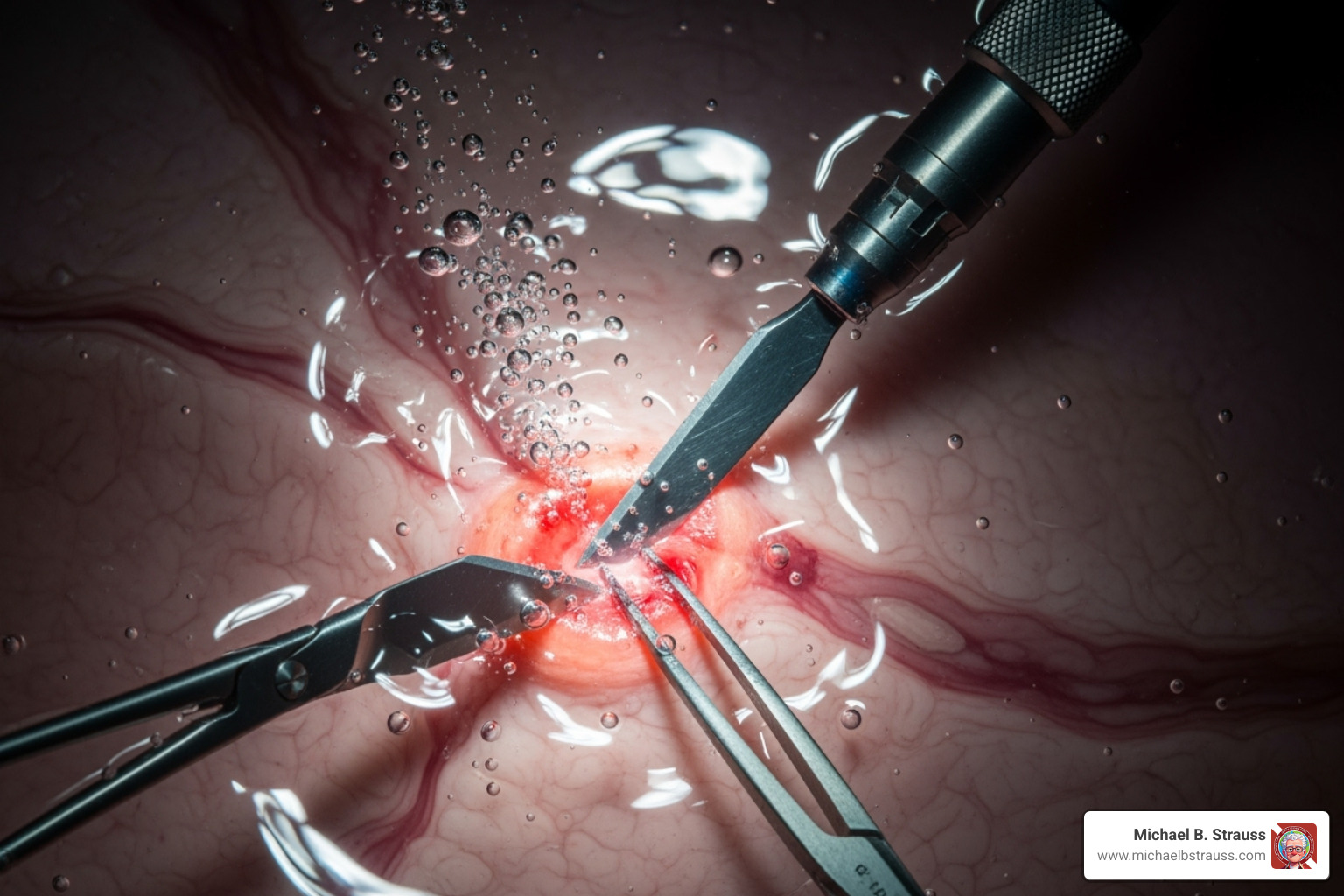
U-ESD performs the entire dissection underwater, offering remarkable advantages. The clearer surgical field is a key benefit, as smoke and debris from electrocautery virtually disappear. The surrounding water also acts as a heat sink, minimizing thermal damage to deeper layers, which is crucial in delicate areas like the esophagus.
The fluid environment also helps with tissue stabilization, allowing for more controlled dissection. The evidence, while growing, is promising. For gastric lesions, studies show U-ESD achieves shorter procedural times with similar en-bloc resection rates compared to standard techniques. Esophageal and colorectal applications also show promising results, with some series reporting 100% en-bloc rates and lower complication rates.
However, we must acknowledge evidence gaps. More robust studies are needed to fully understand U-ESD's potential and long-term outcomes across different anatomical locations.
The SCUBA Technique: Underwater Neurosurgery for Brain Hemorrhage
Moving from the digestive system to the brain, the SCUBA technique (Stereotactic Intracerebral Hemorrhage Underwater Blood Aspiration) applies underwater principles to neurosurgery.
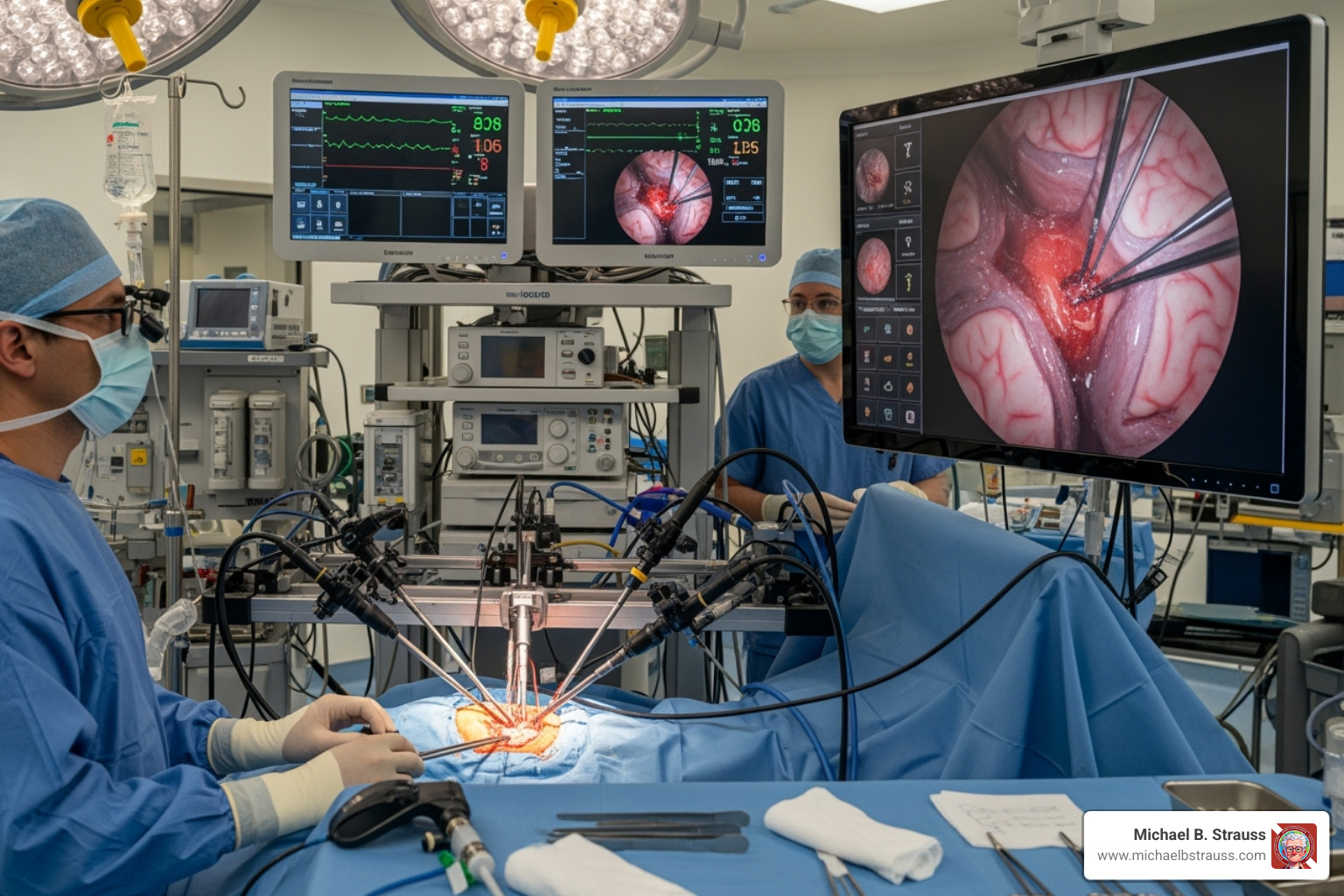
When a brain hemorrhage occurs, blood clots create dangerous pressure. The SCUBA technique addresses this in two phases. First, a dry-field phase involves inserting a tube to suction out the liquid parts of the clot.
Then, in the underwater phase, the cavity is filled with saline, creating a clear surgical environment. This continuous irrigation allows surgeons to see remaining clot fragments and immediately identify any active bleeding, which appears as a visible plume in the clear fluid.
Active bleeding management becomes highly effective. Surgeons can pinpoint the source and use electrocautery to seal it while maintaining perfect visibility.
Clinical results from a study of 47 patients are impressive, with an average evacuation percentage of 88.2%—well above the 70% threshold associated with better outcomes. Active bleeding was observed in 48.9% of cases but was successfully controlled. Complication rates were low, with intraoperative bleeding at 6.4% and postoperative re-bleeding at just 2.1%. The SCUBA technique shows how underwater principles can be adapted to improve patient outcomes across different specialties.
Scientific research on the SCUBA technique
Navigating the Challenges and Future of Underwater Surgery
Even pioneering techniques have challenges. Here are the current limitations of underwater surgery.
Current Limitations and Risks of Underwater Surgery Techniques
Fluid-related complications are a primary concern. Large fluid volumes can lead to fluid overload or hyponatremia (low blood sodium) if sterile water is absorbed. For this reason, most surgeons prefer isotonic saline.
In neurosurgery, increased intracranial pressure (ICP) is a unique risk that requires careful monitoring. Scientific research on irrigation and ICP continues to guide best practices in this delicate area.
The technical learning curve is also significant. Surgeons must adapt to working in a fluid environment where instruments behave differently.
Finally, a lack of standardization and the need for more specialized equipment are problems that are being addressed as the techniques evolve.
The Next Wave: Emerging Applications like U-POEM and U-EFTR
The success of established techniques has sparked innovation. Two exciting developments are U-POEM and U-EFTR.
U-POEM (Underwater Peroral Endoscopic Myotomy) is an emerging treatment for achalasia, a swallowing disorder. Performing the muscle-cutting procedure in a fluid-filled environment may offer clearer visualization and reduce thermal damage. Early case reports are promising, but larger trials are needed.
U-EFTR (Underwater Endoscopic Full-Thickness Resection) tackles the complex removal of lesions that go through the entire GI tract wall, such as certain gastrointestinal stromal tumors (GISTs). The underwater approach may offer better visualization for these intricate procedures. Like U-POEM, U-EFTR is still in the early stages and requires more extensive study to establish safety and efficacy.
These emerging applications show how underwater surgery techniques continue to expand into new territories.
Conclusion: The Rising Tide of Surgical Innovation
Underwater surgery techniques represent a paradigm shift in minimally invasive surgery. From the buoyant tissue lifting of U-EMR to the clear visualization of U-ESD and the life-saving precision of the SCUBA technique, these methods are fundamentally improving complex procedures.
The results—higher success rates for polyp removal, shorter procedure times for gastric lesions, and 88.2% clot evacuation rates in brain surgery—demonstrate real improvements in patient care.
While challenges like learning curves and fluid management exist, the future looks bright. As more surgeons master these methods and equipment improves, applications will expand. Cross-specialty collaboration will likely accelerate innovation.
Training and education are crucial for this surgical revolution. Mastering any complex underwater environment requires dedication, proper instruction, and respect for the unique challenges involved.
Speaking of mastering complex underwater environments, Dr. Michael B. Strauss brings decades of expertise in diving safety and the intricate relationship between humans and challenging fluid environments. His comprehensive approach to safety and scientific understanding makes his work invaluable.
Whether you're fascinated by surgical innovation or passionate about diving safety, the principles of understanding pressure, respecting fluid dynamics, and prioritizing safety remain constant.
Get your copy of Diving Science Revisited today!
DISCLAIMER: Articles are for "EDUCATIONAL PURPOSES ONLY", not to be considered advice or recommendations.






